In times when making it out alive is based on luck, getting tested for coronavirus has become an essential tool to save lives. The unavailability of enough kits and inefficacy of swab tests has made the prospects of living grimmer. If someone’s test result is negative, it does not always mean the absence of infection in the body.
Proactive approaches of testing for Covid-19 in communities can prove to be an effective way to address the problem. Examining the presence of Covid-19 in wastewater is a promising way to forecast future surges. In order to make this method a success and to determine potential environmental transmission routes, it is imperative to know the active time of coronavirus in water and wastewater. In tap water, coronavirus can survive up to 10 and 100 days at 23°C and 4°C respectively. Similarly, according to published research, coronavirus persists in wastewater for two to four days at 23°C.

source: Dutch water sector.
Detecting problems in a locality via wastewater is not a thing of the future.Wastewater-based epidemiology has been used for many years to determine the activities of inhabitants, including use of illicit drugs within the community by collecting quantitative and qualitative data of contaminants. This technique was first proposed in 2001 and applied in 2005. The future applications of this tool of surveillance can also be to monitor diet habits, disease patterns and exposure to environmental and food contaminants in neighbourhoods.
In these uncertain times, it is imperative to have timely and targeted testing for coronavirus to know when it is safe to re-open communities. For this, wastewater-based epidemiology (WBE) is now being applied to detect coronavirus in communities. This method is cost-effective and ensures the early detection of the virus as compared to individual testing. Individual or diagnostic testing is not only fickle, but also it does not warn us about the future surges of the epidemic. Furthermore, not everyone can get tested for coronavirus; some cannot afford it, and some choose not to get tested. Wastewater-based epidemiology (WBE) detection is based on enumerating the virus RNA (ribonucleic acid) in sewage and performing mass balance approach on virus shedding using population and sewage flow rate. While this holistic job of detection can predict the number of patients, it cannot tell the individual identity of the patient.
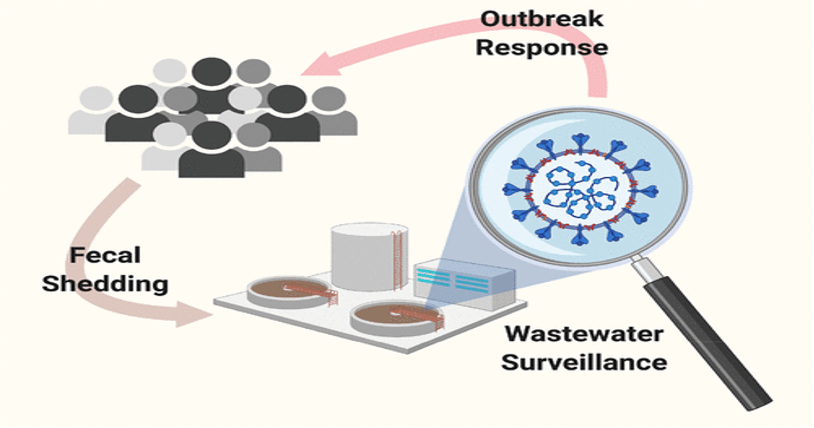
Source:(Wastewater-Based Epidemiology: Global Collaborative to Maximize Contributions in the Fight Against COVID-19)
Using this method, it has become feasible to know the number of coronavirus cases in a locality. According to reports, coronavirus was found to be in sewage of Spain and Italy, before the first case was prevailed in China. Scientists claim that when the virus was detected last year, it was less contagious but mutated into a more harmful form afterwards. This could be the reason that it took so long to detect coronavirus in Europe. Globally, it is now becoming the new normal to test for the virus in wastewater as researchers in Netherlands, Australia, France, Sweden, and USA have confirmed the presence of the virus in wastewater.
Inspired by the potential of this research, MIT alumni Mariana Matus launched BIBOT Analytics. This start-up is working hard to make wastewater treatment facilities as public health observatories. Here, wastewater samples are pasteurized at 60°C for sixty minutes to make the sample safe for handling. BIBOT is working with 400 wastewater facilities across the Unites States of America to help update the healthcare database system.
Even though, there is no question on the authenticity of this tool of surveillance, still, there are challenges in this area. True quantitative assessment of coronavirus patients is ambitious because there are a number of factors involved and there is variability in these factors. One of the factors is the uncertainty in virus shedding rates between people at different stages of infection. Other factors include the time of persistence of viral RNA in wastewater and flow variations of sewage.
Despite being a useful tool for the management of Covid-19 in communities, sewage may be a route of transmission of Covid-19 in people. Coronavirus can survive in different media with varying life spans. This information is critical because of the airborne transmission of the virus; it poses a serious question of infection due to wastewater aerosols. Right now, there is no inclusive data that declares this as a substantial health risk. However, there are several routes of transmission that are possible, which include environmental surfaces, aerosols, and faecal-oral route. Respiratory route is well-known but credibility of other routes of transmission is still a question in research.
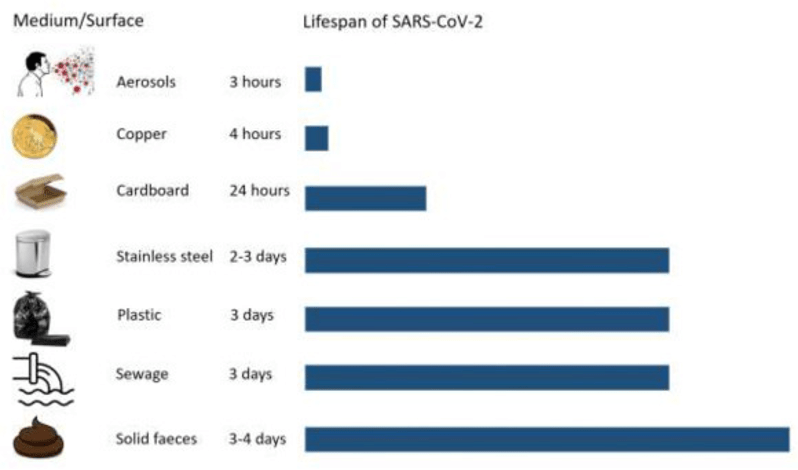
Source: Elsevier Public Health Emergency Collection
Wastewater-based epidemiology (WBE) for coronavirus is showing a promising future in handling the situation of the pandemic across globe. As the world is trying to reopen, academic institutions are looking forward to collecting data of virus transmission from student apartments’ sewage. This will help them in controlling the situation by devising plans intermittently according to the existing condition of pandemic. Advancements are happening at a fast pace and in order to estimate the exact population size and to discover new methods of biomarker extraction, research has to be conducted to improve the outcomes of this surveillance tool.




Very well written…..